Is Niacinamide Bad for Rosacea? Dermatologist Recommended Guide in 2026
If you have rosacea, you’ve probably heard conflicting advice about niacinamide. One dermatologist says it’s a lifesaver. A Reddit thread says it torched someone’s skin. And somewhere in the middle, you’re standing at the drugstore staring at a serum bottle, completely confused. Sound familiar?
Here’s the truth: niacinamide is one of the most widely studied topical ingredients for rosacea-prone skin — and for the vast majority of people, it works beautifully. But nuance matters. According to the National Rosacea Society, over 16 million Americans live with rosacea, and managing it requires precision — particularly when it comes to skincare actives.
In this article, I’m breaking it all down.
Is niacinamide actually bad for rosacea?
What does the clinical evidence say?
What concentration should you use, and when could it cause a flare-up?
I’ll also cover the gut-skin axis connection (yes, SIBO and rosacea are linked!), the best Korean skincare ingredients for rosacea, and how to build a complete rosacea-safe routine.
Let’s get into it.
What Rosacea Actually Is — And Why Your Skin Barrier Matters More Than You Think
Rosacea isn’t just flushing easily or having “sensitive skin.” It’s a chronic inflammatory condition that alters how your skin behaves at a cellular level — making it reactive to stimuli that wouldn’t register for most people. Understanding what’s happening underneath the surface matters more than any single product choice you’ll ever make.
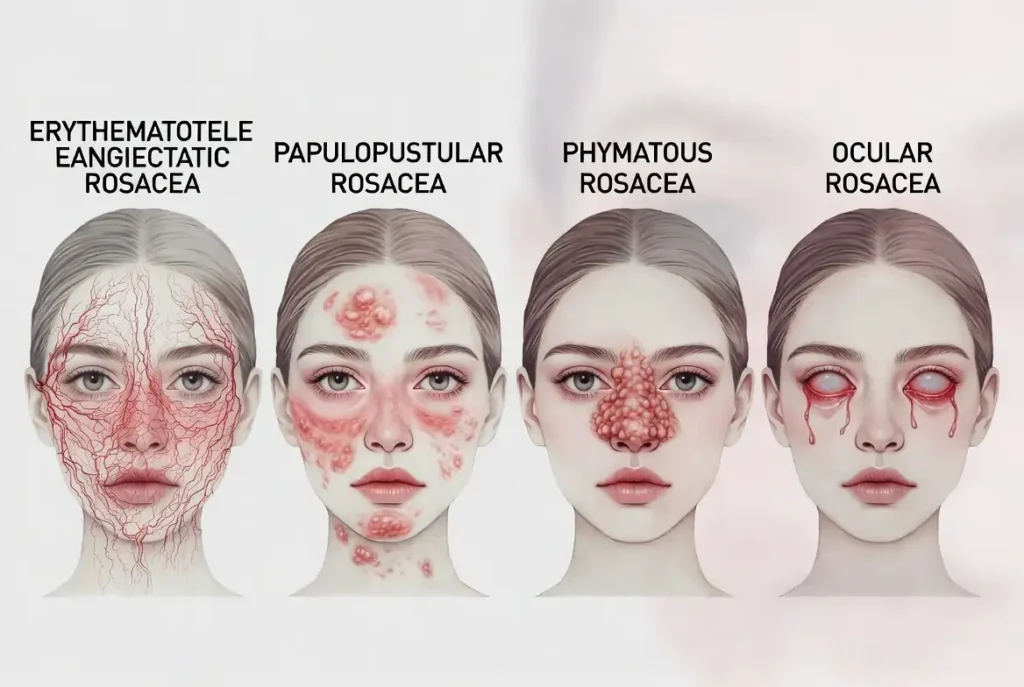
There are four distinct types, and confusing them leads to the wrong routine
The four subtypes are erythematotelangiectatic rosacea (chronic redness and visible blood vessels), papulopustular rosacea (inflamed bumps often misidentified as acne), phymatous rosacea (skin thickening, more common in men), and ocular rosacea (eye dryness and sensitivity). According to clinical guidance from the American Academy of Dermatology, identifying your specific subtype is essential before building any management routine — because the same product that helps one type can meaningfully aggravate another.
Papulopustular rosacea, for instance, is frequently mistaken for adult acne and treated with benzoyl peroxide or salicylic acid — both of which can worsen inflammation in rosacea-prone skin significantly. Getting the diagnosis right first isn’t just pedantic; it’s the difference between progress and months of backsliding.
A compromised skin barrier keeps rosacea locked in a cycle
Rosacea skin has a structurally weakened epidermal barrier — one that loses moisture faster and absorbs irritants more readily than healthy skin. This creates a self-reinforcing loop: irritation damages the barrier further, which makes the skin more reactive, which triggers more inflammation.
Niacinamide’s ability to meaningfully strengthen this barrier is central to why it’s increasingly recommended in rosacea management, according to clinical analysis from the Melbourne Skin & Dermatology Clinic.
What Is Niacinamide — And Why Do Dermatologists Keep Recommending It?
Niacinamide is a water-soluble form of vitamin B3. Your body can’t produce it on its own — you get it through diet or topical application. Once it’s in your skin, it does a surprising number of things simultaneously, which is exactly why it’s earned the “multitasking ingredient” reputation it can’t seem to shake.

The ceramide-building, cytokine-calming mechanism behind niacinamide
When applied topically, niacinamide stimulates ceramide production — the lipids responsible for sealing moisture in and keeping irritants out of the skin. It also modulates pro-inflammatory cytokines, the chemical messengers that drive the immune overreaction at the heart of rosacea.
This dual action — barrier repair alongside active anti-inflammation — makes it genuinely useful for reactive skin. According to the Melbourne Dermatology Clinic, niacinamide also inhibits the specific chemical triggers responsible for vasodilation, which directly reduces the flushing that rosacea patients find most disruptive.
A quick tangent worth knowing: niacinamide isn’t just a skincare ingredient. It’s also being studied as an oral supplement. Research published in the New England Journal of Medicine found that 500mg of oral niacinamide twice daily reduced non-melanoma skin cancers by 23% over 12 months. That’s a different application — and a significantly higher dose than you’d get from any topical — but it speaks to how broadly this molecule affects skin biology.
For rosacea management, topical application at an appropriate concentration remains the most studied and recommended route.
Is oral niacinamide different from topical, and does it matter for rosacea?
Yes, the distinction matters. Topical niacinamide works locally at the skin surface; oral niacinamide has systemic effects. For rosacea specifically, initial studies on oral niacinamide are showing promise, but the Melbourne Dermatology Clinic notes that more research is needed before it can be formally recommended as a primary rosacea treatment.
What’s well-established is that topical niacinamide at the right concentration consistently improves rosacea symptoms — redness, dryness, barrier function — across multiple clinical trials. That’s where the confidence is.
Is Niacinamide Bad for Rosacea? Here’s What the Research Actually Shows
Short answer: no — not for most people. But the full answer carries nuance that matters, particularly if you’ve tried niacinamide before and had a reaction. The difference between an ingredient problem and a formulation problem is something a lot of skincare conversations get badly wrong.
The clinical trial that made dermatologists take niacinamide seriously for rosacea
A randomized, investigator-blind controlled study (N=50) published on PubMed had rosacea patients apply a niacinamide-containing facial moisturizer twice daily for four weeks.
Results showed measurable improvements in stratum corneum barrier function alongside clinical reductions in redness, dryness, and flakiness. This isn’t an isolated finding — multiple subsequent studies have replicated similar outcomes.
Dr. Fricke of Alamo Heights Dermatology notes specifically that niacinamide’s “soothing and anti-inflammatory effects can alleviate the redness and irritation associated with rosacea”.
In a separate analysis reviewed by PrettyBoy, one study found that 76% of participants using a niacinamide gel moisturizer twice daily for four weeks experienced a meaningful reduction in rosacea symptoms. Those are not small numbers.
When niacinamide does cause a reaction — what’s actually going on?
Here’s where the conversation gets important. Rosacea skin has a compromised barrier, which means it can react to almost anything — even genuinely gentle ingredients.
Higher concentrations of niacinamide, particularly at 10% and above, can overwhelm sensitive skin and trigger redness, burning, or stinging. This doesn’t automatically mean niacinamide is the culprit. It usually means the concentration was too high, introduced too quickly, or the product contained other irritating ingredients alongside it.
Natural Image Skin Center puts it directly: “niacinamide’s stimulation of the skin’s immune response — usually beneficial — can actually exacerbate redness and stinging in rosacea-prone skin” at high concentrations.
The solution isn’t to abandon niacinamide. It’s to use less of it.
The nicotinic acid flushing problem — a formulation issue, not an ingredient issue
Some people experience visible flushing after applying niacinamide products — and it’s almost never the niacinamide itself causing it. Impure or poorly manufactured products can contain elevated levels of nicotinic acid (niacin), which causes vasodilation and flushing, according to a clinical analysis by Biology Insights. This is a quality control issue.
Choosing products from brands with transparent formulation standards and third-party testing largely eliminates this reaction for most people. If you’ve had a “niacinamide reaction” before, this is likely what you were actually responding to.
How to Use Niacinamide Safely When You Have Rosacea
The most common mistake rosacea patients make with niacinamide is starting at the highest concentration they can find, reasoning that more potency means faster results. That logic works poorly for reactive skin. Your skin doesn’t need 10% right out of the gate. It needs a patient introduction — the same kind of slow build you’d apply to any powerful topical.
Start at 2–5% and build gradually — here’s the clinical reasoning
A moisturizer containing just 2% niacinamide showed clinically meaningful reductions in rosacea symptoms — blotchiness, flakiness, papules — after four weeks of use, per the Melbourne Dermatology Clinic’s clinical overview. That is a low concentration producing genuine, documented results.
SkinGPT’s rosacea-specific guidance recommends starting every other day before building to daily use — a gradual approach that gives reactive skin time to adapt without triggering a flare.
A sample AM/PM routine for rosacea-prone skin featuring niacinamide
Here’s a framework aligned with dermatologist-supported guidance. The morning routine prioritizes barrier protection and mineral sun defense. The evening routine focuses on active rosacea management. Fewer products mean less combined irritation risk — for rosacea skin, simplicity is a genuine clinical strategy, not just minimalism for its own sake.
| Step | Morning | Evening |
|---|---|---|
| 1 | Gentle, low-pH cleanser | Gentle, low-pH cleanser |
| 2 | 2–5% Niacinamide serum | Azelaic acid (alternate nights) |
| 3 | Ceramide-rich moisturizer | 2–5% Niacinamide moisturizer |
| 4 | Mineral SPF 30+ (non-negotiable) | Heavier barrier cream if needed |

Not all mineral sunscreens are created equal for rosacea skin — if you’re not sure which zinc oxide formula won’t irritate your face, we’ve broken down the best options in our zinc oxide sunscreens for rosacea guide.
UV exposure is one of the most consistent rosacea triggers. Daily broad-spectrum mineral sunscreen — zinc oxide or titanium dioxide-based — isn’t optional for rosacea management.
What to safely pair with niacinamide — and what to keep separate
Niacinamide plays well with azelaic acid (dermatology’s preferred rosacea combination), ceramides, hyaluronic acid, panthenol, and centella asiatica — all of which complement its barrier-repair and anti-inflammatory effects. Use real caution with retinoids: introduce them separately under dermatologist guidance, never stacked with niacinamide at first.
Avoid combining niacinamide with high-strength vitamin C serums or exfoliating acids during active flares — the chemical load on a reactive, compromised barrier is simply more than rosacea skin can process without responding badly.
Niacinamide vs. Other Rosacea Ingredients: What Actually Works?
No ingredient exists in isolation. Understanding how niacinamide compares to — and works alongside — other commonly recommended actives helps you build a routine that addresses what rosacea is actually doing, rather than just adding products and hoping something sticks.
Is niacinamide or hyaluronic acid better for rosacea?
They do different jobs, which is why most dermatologists recommend both. Niacinamide actively reduces inflammation and boosts ceramide levels. Hyaluronic acid is a humectant that draws moisture into the skin.
Some rosacea patients find high-molecular-weight HA mildly irritating in dry climates; low-molecular-weight sodium hyaluronate tends to be better tolerated. Used together, they form a solid hydration-plus-inflammation foundation for any rosacea routine.
Niacinamide and azelaic acid — dermatology’s most-recommended rosacea combination
Azelaic acid (15–20% by prescription, or lower OTC concentrations) holds FDA-approved status for rosacea treatment. It reduces inflammation, manages papulopustular breakouts, and gently encourages cell turnover without the stripping risks of traditional exfoliants.
Combined with niacinamide, the two address different inflammatory pathways simultaneously, per the clinical analysis referenced by PrettyBoy. Using them on alternating evenings or a morning-versus-evening split is a practical, widely used approach that dermatologists regularly recommend.
If you’re also dealing with acne alongside rosacea, the two ingredients work differently on breakouts too — we’ve compared them head-to-head in our full niacinamide vs. azelaic acid for acne breakdown.
Can you use bakuchiol if you have rosacea?
Yes — and for rosacea patients who want retinol-like anti-aging results without the associated irritation, bakuchiol is a genuinely better starting point than traditional retinoids. Derived from the Psoralea corylifolia plant, it delivers cell-turnover benefits with a significantly gentler profile.
It won’t address active rosacea inflammation on its own, but it’s compatible with a rosacea-safe routine and carries minimal risk of triggering the kind of reactive flares that traditional retinol frequently causes in sensitive skin.
The Skincare Ingredients That Make Rosacea Genuinely Worse
Some of the most widely used skincare actives are among the worst possible choices for rosacea skin. Knowing what to put down is just as strategically important — possibly more so — as knowing what to pick up. These aren’t opinions; they’re patterns documented repeatedly across clinical dermatology.
Fragrance is the single biggest rosacea trigger in skincare — and it hides everywhere
Fragrance — synthetic or labeled “natural” — is one of the most consistently documented topical sensitizers for rosacea-prone skin. It appears under labels like parfum, essential oils, and specific chemical compounds like linalool or citronellol.
The Korean rosacea skincare protocol from Koreancare lists fragrance avoidance as its first principle of rosacea-safe formulation. Check every INCI list carefully — the ingredient most responsible for your flares might be the one you’d least suspect.
Beyond fragrance, the standard avoid list for rosacea includes: alcohol denat., witch hazel, menthol, camphor, benzoyl peroxide, high-concentration glycolic or salicylic acid during flares, physical scrubs, sodium lauryl sulfate (SLS) in cleansers, and oxybenzone-based chemical sunscreens.
Mineral sunscreens with zinc oxide are the recommended alternative — zinc oxide is actually mildly anti-inflammatory, which makes it unusual among SPF options.
The Gut-Skin Connection — Is Your Rosacea Actually a Gut Problem?
This is the part of rosacea management that most skincare routines never touch. And it might explain why some people’s rosacea doesn’t respond the way it should — even with the right products, a disciplined routine, and real commitment.
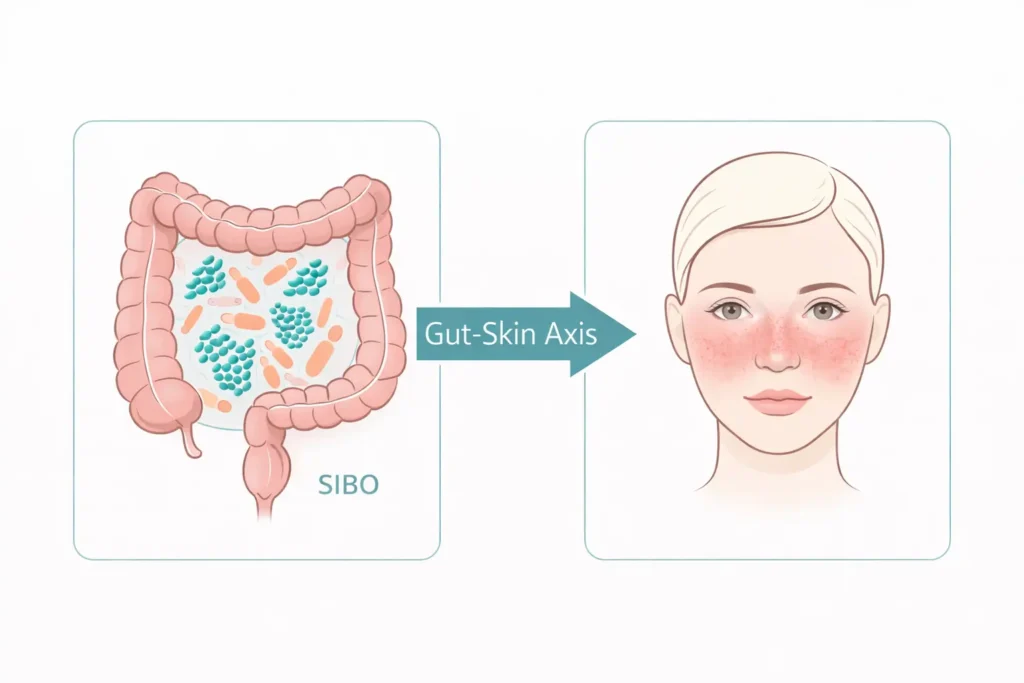
What the SIBO-rosacea research actually shows — and what it means for your skin
A 2024 Mendelian randomization study published in Frontiers in Medicine confirmed a causal relationship between gut microbiota composition and rosacea. Small intestinal bacterial overgrowth (SIBO) has been found in rosacea patients at a prevalence up to 13 times higher than in the general population, per FoodMarble‘s clinical summary.
In one clinical trial, treating SIBO with rifaximin led to a 78% improvement in skin lesions, with 96% of patients in remission remaining symptom-free for at least nine months, according to OMED Health.
The mechanism runs through the gut-skin axis. SIBO increases intestinal permeability — sometimes called “leaky gut” — which allows bacterial components and pro-inflammatory cytokines to enter systemic circulation. That systemic inflammation then manifests at the skin surface. It’s one of the more striking examples of how skin conditions can have roots far outside the skin itself.
Dr. Marvin Singh, an integrative gastroenterologist and founder of Precisione Clinic, states: “We know that data shows a higher prevalence of rosacea in those with SIBO, and that treatment of SIBO could possibly result in an improvement in rosacea.”
If your rosacea is persistent despite a solid topical routine, it might be worth discussing a hydrogen-methane breath test with a gastroenterologist. It’s non-invasive, relatively inexpensive, and could genuinely change your treatment direction. The American Academy of Family Physicians notes the evidence is promising, though they recommend professional medical evaluation before pursuing SIBO treatment specifically for rosacea.
What Koreans Use for Rosacea — And What Makes K-Beauty Different
Korea’s skincare philosophy has attracted real global attention in the context of rosacea management. And it’s not simply marketing. The core principles behind K-beauty’s formulation choices align remarkably well with what clinical dermatology recommends for compromised, reactive skin — and it’s worth understanding why.

The K-beauty ingredients that genuinely earn their place in a rosacea routine
Centella asiatica (CICA, or tiger grass) is rich in madecassoside and asiaticoside — compounds with well-documented anti-inflammatory properties and barrier-strengthening effects. Mugwort offers cooling, anti-inflammatory benefits particularly suited to flushing and redness.
Heartleaf (houttuynia cordata), the hero ingredient in Anua’s Heartleaf 77% Soothing Toner, delivers concentrated calming actives without synthetic irritants. Ceramides, panthenol, and low-dose niacinamide complete the core K-beauty rosacea framework, per the DK Blog’s 2025 ingredient roundup.
The K-beauty structural philosophy also matters: layered lightweight hydration instead of single heavy creams, fragrance-free and alcohol-free formulations as standard, and products calibrated to a slightly acidic pH of around 5.5 — which matches the skin’s natural environment and doesn’t disrupt its microbiome.
Popular products with strong clinical ingredient profiles for rosacea include: SKIN1004 Madagascar Centella Asiatica Ampoule, I’m From Mugwort Essence, Beauty of Joseon Glow Serum (60% propolis + 2% niacinamide), and the Round Lab Birch Juice Moisturizing Sunscreen. These aren’t magic — but their ingredient lists are genuinely thoughtful for reactive skin.
Is rosacea common in Korea?
Less so than in Western populations. Prevalence estimates put rosacea at approximately 2–3% in East Asian populations compared to 10% in Caucasians — a difference likely rooted in genetics and skin microbiome variation.
When it does occur in Korean patients, it’s often harder to diagnose because redness is less visually pronounced in deeper skin tones. Korean dermatology clinics in Seoul (including Wonjin Beauty Medical Group and Banobagi) offer professional laser treatments for rosacea alongside topical management.
What Calms a Rosacea Flare-Up Fast?
When a flare hits, the instinct for most people is to reach for more products. That’s usually the wrong move. Active flares are your skin’s signal to strip things back — not layer up. The goal during a flare is immediate calm, not active treatment.

The first 24 hours:
Apply a cool (never ice-cold) compress to reduce vascular flushing. Cut your routine to a gentle low-pH cleanser and a plain ceramide moisturizer — nothing else. Don’t exfoliate. Don’t exercise intensely. Don’t use heat on your face.
Ingredients that genuinely calm rosacea quickly:
- Centella asiatica / madecassoside — the most consistent botanical calming agent in the clinical literature
- Colloidal oatmeal — well-documented anti-inflammatory and barrier-supporting properties
- Panthenol (vitamin B5) — hydrates and reduces surface inflammation simultaneously
- Aloe vera (pure, fragrance-free only) — cooling and mildly anti-inflammatory
- Low-dose niacinamide (2–4%) if you’ve already established tolerance
From the inside out: Reducing alcohol and spicy food intake during a flare, managing stress (a genuine trigger via cortisol-driven vasodilation), and staying well-hydrated are all clinically relevant lifestyle strategies.
When to see a dermatologist: If flare-ups are frequent, spreading beyond the central face, or accompanied by eye symptoms — that’s ocular rosacea, and it needs medical attention. Prescription options including metronidazole, ivermectin (Soolantra), brimonidine gel, and low-dose oral doxycycline exist specifically for rosacea management and are meaningfully more effective than topical skincare alone for moderate-to-severe cases.
Conclusion: Is Niacinamide Bad for Rosacea?
Here’s the honest summary: niacinamide is not bad for rosacea. For most people, it’s one of the more clinically defensible topical ingredients available — anti-inflammatory, barrier-building, ceramide-stimulating, and well-tolerated at the right concentration. The issue isn’t niacinamide. The issue is usually concentration (starting too high), product purity (impure formulas with nicotinic acid residue), or formulation (other irritants riding along for the trip).
Start at 2–4%. Patch test. Give it four weeks before making any judgment.
And if you’ve done everything right topically — the gentle routine, the mineral SPF, the fragrance-free everything — and your rosacea still keeps flaring? Consider looking further inward. Literally. The SIBO-rosacea connection isn’t fringe research anymore. It’s published in peer-reviewed journals, replicated across multiple studies, and increasingly discussed in dermatology. Your skin might be telling you something your digestive system needs to hear.
Rosacea is chronic. That’s genuinely frustrating, and it’s okay to feel that frustration. But it’s also manageable — especially when you stop treating the surface and start treating the full system. Consult a board-certified dermatologist if you haven’t already. A professional assessment, even just one, changes the quality of every decision you make after it.
Frequently Asked Questions: Is Niacinamide Bad for Rosacea?
Can niacinamide make rosacea worse?
In some cases, yes — particularly at high concentrations (10%+) or in poorly formulated products containing elevated nicotinic acid. Rosacea-prone skin can react with redness, stinging, or burning even to gentle ingredients. Clinical evidence, however, strongly supports 2–5% niacinamide as beneficial. If you experience persistent irritation, lower the concentration and patch test before reapplying.
Is niacinamide or hyaluronic acid better for rosacea?
Neither is strictly better — they address different needs. Niacinamide reduces inflammation and builds ceramides. Hyaluronic acid hydrates. Most dermatologists recommend using both. If standard HA causes irritation, switch to low-molecular-weight sodium hyaluronate, which penetrates more efficiently and is generally better tolerated by reactive skin.
What ingredients should you avoid if you have rosacea?
Avoid fragrance/parfum, alcohol denat., witch hazel, menthol, camphor, benzoyl peroxide, high-strength glycolic or salicylic acid during flares, physical exfoliants, SLS in cleansers, and oxybenzone-based chemical sunscreens. During active flares, pause all exfoliating acids regardless of concentration and strip your routine back to essentials only.
What do Koreans use for rosacea?
Key K-beauty ingredients for rosacea include centella asiatica, mugwort, heartleaf extract, propolis, ceramides, panthenol, and low-dose niacinamide. Top products include SKIN1004 Madagascar Centella Ampoule, Anua Heartleaf 77% Soothing Toner, I’m From Mugwort Essence, and Beauty of Joseon Glow Serum. Korean clinics in Seoul also offer professional laser and topical prescription treatments.
What serum should you not use if you have rosacea?
Avoid serums with high-dose vitamin C (L-ascorbic acid at pH below 3.5), fragrance, alcohol, witch hazel, and high-concentration AHAs during flare periods. Retinol serums need dermatologist guidance for rosacea skin. Any new serum — regardless of how gentle it’s marketed — should be patch tested on the inner arm for 48–72 hours before facial application.
What calms down a rosacea flare-up?
Apply a cool compress, simplify your routine to a gentle cleanser plus plain ceramide moisturizer, and avoid all actives. Centella asiatica, panthenol, aloe vera, and colloidal oatmeal are the most reliably calming topical ingredients. Reduce alcohol, spicy food, stress, and direct heat exposure. If flares are frequent or severe, consult a board-certified dermatologist about prescription options.
Should I avoid hyaluronic acid if I have rosacea?
Not necessarily. Most dermatologists consider HA a good hydration choice for rosacea. However, some patients with reactive skin find high-molecular-weight HA mildly irritating in dry environments, where it can pull moisture from the skin. Try low-molecular-weight sodium hyaluronate instead, and always seal it with a ceramide moisturizer to prevent transepidermal water loss.
What ingredients make rosacea worse?
Fragrance is the most documented culprit. Beyond that: alcohol denat., witch hazel, menthol, high-strength essential oils, benzoyl peroxide, aggressive exfoliating acids, and nicotinic acid in impure niacinamide formulations. Even hot water during cleansing and physical scrubs qualify — rosacea skin is reactive to mechanical and thermal triggers as much as chemical ones.
Is rosacea linked to SIBO?
Yes — significantly. Research published in Frontiers in Medicine (2024) confirmed a causal relationship between gut microbiota and rosacea. People with rosacea are up to 13 times more likely to have SIBO. Treating SIBO with rifaximin produced a 78% improvement in skin lesions in one clinical trial. The gut-skin axis is a real and clinically relevant connection for rosacea patients.
Can you use bakuchiol if you have rosacea?
Yes. Bakuchiol is plant-derived and provides retinol-like anti-aging benefits with significantly less irritation risk. It’s compatible with rosacea-safe routines and unlikely to trigger flares when introduced gradually. It won’t resolve active rosacea inflammation on its own, but it’s a genuinely sensible option for patients who want anti-aging effects without retinoid-associated reactivity.
What Korean skincare is good for rosacea?
Products with centella asiatica, heartleaf, mugwort, ceramides, and low-dose niacinamide. Standouts include SKIN1004 Madagascar Centella Asiatica 100 Ampoule, Anua Heartleaf 77% Soothing Toner, I’m From Mugwort Essence, Dr. Jart+ Cicapair Tiger Grass Serum, and Round Lab Birch Juice Moisturizing Sunscreen. Always choose fragrance-free, alcohol-free formulations with short INCI lists.
How do Asians deal with rosacea?
Asian approaches to rosacea prioritize gentle barrier repair over aggressive treatment — using cooling botanicals like centella, green tea, and mugwort alongside ceramides and layered lightweight hydration. Modern Korean and Chinese dermatology also uses laser treatments (IPL, pulsed dye laser) alongside prescription topicals. The skin-first, minimal-irritation philosophy of K-beauty aligns naturally with rosacea management principles.
Is rosacea common in Korea?
Less so than in Western countries. Prevalence is estimated at approximately 2–3% in East Asian populations versus around 10% in Caucasian populations — a difference likely related to genetics and skin microbiome variation. Rosacea in Korean patients is often underdiagnosed because visible redness is less apparent in deeper skin tones. Korean dermatology clinics in Seoul are well-equipped with both topical and laser treatment options for those who are affected.
📋 Medical Disclaimer
For Educational Purposes Only: This article is written by Kousar Subhan, a Medical Writer and Researcher, and is intended for informational and educational purposes only. The content provided is based on scientific research, peer-reviewed studies, and dermatological literature available as of December 2025.
Not Medical Advice: The information in this article does not constitute medical advice, diagnosis, or treatment recommendations. It should not be used as a substitute for professional medical consultation, diagnosis, or treatment from a board-certified dermatologist or qualified healthcare provider.
Individual Results May Vary: Skin conditions, including hyperpigmentation, melasma, and UV-induced pigmentation, vary significantly between individuals based on genetics, skin type, hormonal factors, and environmental exposure.
Consult Your Healthcare Provider: Before starting any new skincare regimen, especially if you are pregnant, breastfeeding, have diagnosed skin conditions, are taking medications, have sensitive skin, or are undergoing dermatological treatments.
Product Safety: Always perform a patch test before using new skincare products. Discontinue use and consult a healthcare professional if you experience irritation or adverse reactions.
🛍️ Affiliate Disclosure
Amazon Associates Program: Glow Guide Hub participates in the Amazon Services LLC Associates Program. When you purchase through our Amazon affiliate links, we may earn a small commission at no extra cost to you.
Editorial Independence: Our affiliate relationships do not influence our content or recommendations. We only recommend products based on scientific research, clinical evidence, and genuine quality assessment.
Supporting Our Mission: Your purchases through affiliate links help us maintain this free, evidence-based educational resource. Thank you for your trust!

