What Is the Skin Microbiome and How to Protect it in 2026: Complete Science-Backed Guide
I spent years thinking healthy skin meant clean skin. Like, really clean. Foam-twice, rinse-three-times, pores-as-smooth-as-glass clean. The tighter my face felt after washing it, the better I thought I was doing. Turns out — I was stripping away the very thing keeping my skin healthy.
Here’s the part that genuinely surprised me. According to research published in Experimental Dermatology, your skin hosts an estimated 1,000 bacterial species, plus fungi, viruses, archaea, and microscopic mites — all living in a complex, highly organized ecosystem. They’ve been there since birth. And the vast majority of them? They’re protecting you.
That ecosystem is your skin microbiome. It’s not a skincare buzzword invented by some marketing department. It’s a living, constantly adapting community of microorganisms that your skin’s barrier, immune system, and pH balance all depend on.
So what happens when it gets disrupted? According to a 2025 review in Microorganisms authored by dermatologists at The Kids Research Institute Australia, imbalance in the skin microbiome — clinically called dysbiosis — is directly linked to eczema, rosacea, persistent acne, and psoriasis. Conditions that, honestly, millions of Americans have been treating symptom by symptom without ever addressing the root cause.
The disruption isn’t always dramatic. It can come from the antibiotic course you took for a sinus infection. The “deep pore cleanser” you bought last year. The fragrance in your daily moisturizer. Small choices with a surprisingly long-lasting impact.
This article covers everything: what the skin microbiome is, what it does, what damages it, and exactly how to protect and restore it. I’ve linked every major claim to a real, verifiable source — because this topic deserves better than vague advice.
Let’s get into it.
What Exactly is the Skin Microbiome?
The skin microbiome is the ecosystem of microorganisms—primarily bacteria, along with fungi and viruses—that live on the surface of your skin and within its upper layers. These microbes aren’t harmful by default; in fact, they play a critical role in protecting the skin, maintaining its barrier, and regulating inflammation.
Think of it as your skin’s built-in defense system. A balanced microbiome helps prevent the overgrowth of harmful bacteria, supports optimal skin pH (around 4.5–5.5), and strengthens the skin barrier to reduce moisture loss and sensitivity.
According to the National Institutes of Health (NIH), these microbial communities are essential for immune function and skin health.
And here’s the part most people don’t expect:
Not all bacteria are bad.
Some of them are essential.
The trillion-organism ecosystem living on your skin right now
According to research published in the Journal of Cosmetic Dermatology in 2024, a single square centimeter of skin contains up to one million microorganisms.
Bacteria are the most abundant group, but fungi, viruses, archaea, and even Demodex mites all share the same real estate. The dominant bacterial phyla — Actinobacteria, Firmicutes, and Proteobacteria — colonize the skin in patterns shaped by the local environment of each body region.
Is your microbiome the same all over your body?
Not even close. A 2024 review in Experimental Dermatology reports that moist zones, such as the armpits and groin, favor Corynebacterium and Staphylococcus species, whereas sebaceous (oily) zones, such as the forehead and back, show higher levels of Cutibacterium acnes. Dry zones, like the forearms, host an entirely different community. Your face, chest, and hands all host distinct microbial communities — each adapted to local pH, humidity, and lipid content.
Your skin microbiome is as unique as your fingerprint
Research published in the Journal of the American Academy of Dermatology confirms that in healthy adults not exposed to antibiotics, the skin microbiome stays remarkably stable over time.
What shapes it?
Your genetics, birth method (vaginal vs. C-section), infant feeding, environment, lifestyle, and the products you apply. It’s genuinely individual — no two people carry the same microbial profile, even in the same household.
What Does A Healthy Skin Microbiome Actually Do For Your Skin Health And Protection??
A healthy skin microbiome functions as an active biological defense system that protects against pathogens, regulates immune responses, and supports long-term skin resilience. It helps maintain barrier integrity, balance inflammation, and even contributes to UV-related cellular protection—making it essential not just for appearance, but for overall skin function and disease prevention.
Your first line of defense against pathogens
Commensal bacteria defend skin territory through what’s called competitive exclusion — they fill ecological niches that harmful bacteria would otherwise occupy. Research published in the Journal of Clinical Investigation describes how specific strains, particularly Staphylococcus epidermidis, produce antimicrobial peptides that directly inhibit pathogens such as S. aureus, which is strongly implicated in eczema flares.
Without a healthy commensal population, there’s less resistance to opportunistic infection. That’s not a subtle difference — it’s significant.
How your skin microbiome and immune system communicate
Regular contact between immune cells and skin microbes regulates cytokine production and the production of antimicrobial peptides. According to the 2024 Experimental Dermatology review, keratinocytes express pattern recognition receptors that distinguish between bacteria, viruses, and fungi — and respond accordingly.
This ongoing two-way communication essentially trains the skin’s immune response to stay calibrated. Disrupt the microbiome, and this calibration slips. Over-reaction (sensitivity, redness) or under-reaction (opportunistic infection) can both follow.
The surprising link between S. epidermidis and UV protection
This one genuinely surprised me when I first read it. Research cited in the JCI review found that S. epidermidis produces a compound called 6-HAP (6-N hydroxyaminopurine) that selectively targets UV-damaged keratinocytes — reducing their proliferation and potentially lowering UV-induced skin cancer risk. Your daily SPF protects both your skin cells and this microbial defense mechanism. That’s a good enough reason to never skip sunscreen again.
If your skin’s own microbes are working to limit UV damage at a cellular level, protecting them with daily sunscreen isn’t optional—it’s essential—learn exactly how to do it right in our complete guide to sun protection and anti-aging.
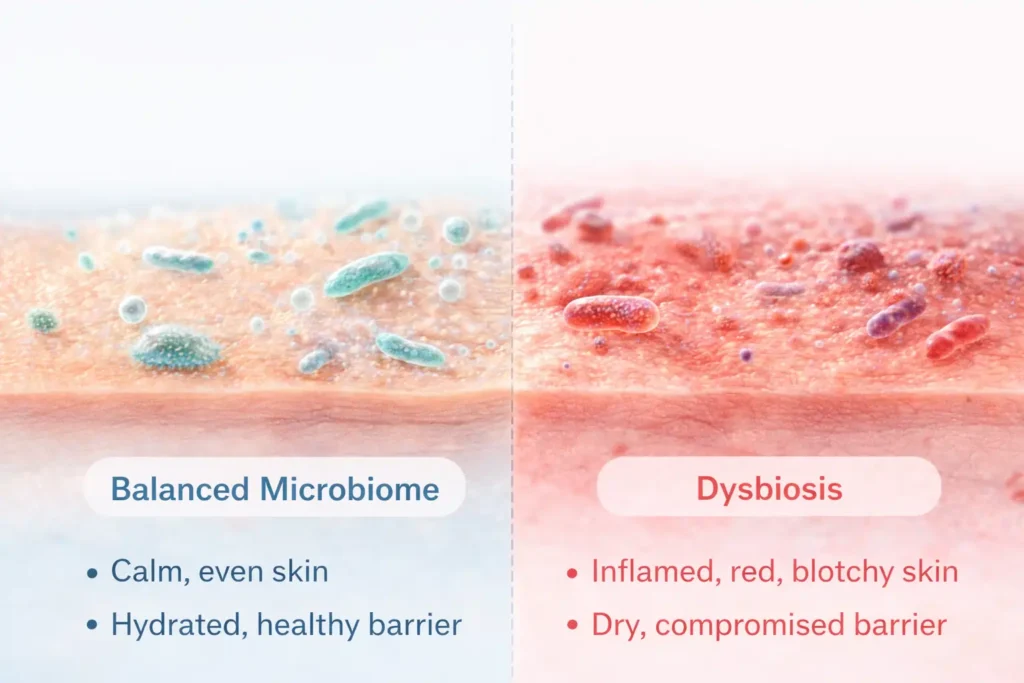
Signs of an Unhealthy Skin Microbiome — Recognizing Dysbiosis
Dysbiosis doesn’t always announce itself with a rash. Sometimes it looks like “bad skin days” that never seem to end. These are the signals worth taking seriously — especially if they’ve persisted despite routine changes.
The symptoms most people mistake for “just bad skin”
A 2025 systematic review in the Journal of Clinical Medicine found that decreased microbiome diversity — not just the presence of pathogens — was a consistent finding across diseased skin. Practically speaking, that looks like: persistent acne that doesn’t respond to standard treatments, skin that feels tight despite regular moisturizing, recurring redness, flaking without a known cause, and a sudden sensitivity to products you’ve used for years without issue. Any of those sound familiar?
Which skin conditions are directly linked to dysbiosis?
The 2025 Microorganisms review identifies atopic dermatitis, rosacea, acne vulgaris, psoriasis, and hidradenitis suppurativa as conditions with a confirmed microbiological component.
In atopic dermatitis, S. aureus overgrowth is almost universal. In seborrheic dermatitis, Malassezia fungi dominate dysregulated skin. In rosacea, Demodex mite overgrowth plays a documented role.
These aren’t coincidences — they’re patterns that researchers are now actively using to develop targeted treatments.
Can chronic stress make your skin microbiome worse?
Yes — and the mechanism is biological, not just anecdotal. A 2024 paper in Microorganisms by Borrego-Ruiz and Borrego documents that persistent dysbiosis is closely associated with anxiety and depression.
Chronic stress alters sebum production, impairs barrier function, and shifts the pH environment that commensal bacteria depend on.
The result is a feedback loop: disrupted microbiome → inflammatory skin response → amplified stress → further disruption. Recognizing that loop is the first step to breaking it.
If stress is already triggering flare-ups or worsening existing skin conditions, understanding that connection more deeply can help you manage both. Explore our guide on how stress affects pre-existing skin conditions and what you can do about it.
What Disrupts the Skin Microbiome? The Biggest Culprits, Ranked
The biggest disruptors of the skin microbiome range from medical treatments like antibiotics to daily habits such as high-pH cleansing, over-exfoliation, and UV exposure. Understanding which factors cause the most long-term imbalance helps you protect beneficial bacteria, maintain barrier function, and prevent chronic skin issues without overcomplicating your routine.
Antibiotics — the most significant and longest-lasting disruptors
A 2021 study from NIH’s NIAMS institute, published in Science Translational Medicine, found that systemic antibiotics cause significant changes to skin microbial communities and — critically — promote the expansion of antibiotic-resistant bacterial strains.
These resistant strains persisted long after the treatment course ended. Both doxycycline and trimethoprim/sulfamethoxazole showed this effect.
This doesn’t mean antibiotics are never necessary; it means their microbiome impact is real, lasting, and worth factoring into treatment decisions.
Your daily face wash might be working against you
High-pH cleansers — particularly traditional bar soaps and foaming washes with sulfates — raise the skin’s surface pH above its natural range of 4.5 to 5.5. That disrupts the acid mantle, which is essentially the pH-regulated habitat that beneficial bacteria need to survive.
According to a 2025 dermatology review at ScienceDirect, chronic overuse of antiseptic washes can select for resistant bacterial strains and permanently shift community composition, even without a full antibiotic course.
Over-exfoliation, UV exposure, and the disruptors hiding in plain sight
Mechanical and chemical exfoliation removes more than dead skin cells — it strips the microbial film living on top of them. UV radiation damages both skin cells and their resident microbes, according to the JCI review.
Add to that: synthetic fragrance (listed as “parfum”), denatured alcohol in toners, triclosan in cleansers, and high-concentration preservatives like methylisothiazolinone — all known to inhibit beneficial skin bacteria. The cumulative effect of these everyday products is often underestimated.
What Kills Good Skin Bacteria? Everyday Skincare Ingredients And Habits That Disrupt Your Microbiome?
Many common skincare habits—especially antibacterial products, alcohol-based toners, synthetic fragrances, and over-exfoliation—can kill beneficial skin bacteria and weaken your microbiome. Understanding these hidden disruptors helps you avoid long-term imbalance, protect your skin barrier, and choose microbiome-friendly alternatives that support healthy, resilient skin instead of stripping it.
Antibacterial products and the collateral damage they cause
A 2024 paper in Dermatology Times on topical antibiotics and antiseptics makes this clear: broad-spectrum antibacterial products kill both harmful and beneficial bacteria without discrimination. During the window of recovery, opportunistic organisms can colonize where commensals used to live.
Daily use of antibacterial soaps on the face — which many people do — creates this cycle repeatedly, never allowing a stable microbial community to re-establish.
Alcohol-based toners, synthetic fragrance, and the acid mantle problem
Denatured alcohol (listed as “alcohol denat.” on labels) is among the harshest leave-on microbiome disruptors in common use. It strips the acid mantle, creating an alkaline surface environment that beneficial bacteria can’t survive in.
Synthetic fragrance — hiding behind the single word “parfum” on ingredient lists — contains hundreds of undisclosed compounds, some of which are directly antimicrobial at concentrations found in leave-on products. These aren’t exotic concerns; they’re in everyday moisturizers, serums, and toners.
The microbiome-safe swap list — a practical reference
| The Disruptor | What It Damages | Microbiome-Safe Swap |
|---|---|---|
| Antibacterial face soap | Wipes out commensals indiscriminately | pH-balanced, sulfate-free gel cleanser |
| Alcohol denat. toner | Destroys the acid mantle | Prebiotic essence or hydrating toner |
| Fragranced daily moisturizer | Inhibits beneficial skin flora | Fragrance-free ceramide cream |
| Triclosan cleanser | Broad-spectrum microbial disruption | Amino acid-based or lactic acid cleanser |
| Daily physical scrub | Strips the microbial surface film | Enzyme exfoliant used 1–2x per week max |
How to Protect Your Skin Microbiome — 7 Strategies That Actually Work
The good news is that protecting your microbiome doesn’t require an expensive routine. It mostly requires stopping certain things — and replacing them with gentler alternatives that support what’s already there.
Strategy 1: Switch to a pH-balanced, sulfate-free cleanser
The skin’s natural pH of 4.5 to 5.5 is not cosmetic preference — it’s a biological necessity for commensal bacteria. A cleanser that raises pH above this range disrupts the acid mantle and makes the skin’s surface inhospitable to beneficial microbes.
Look for labels that say “pH-balanced,” “sulfate-free,” and “fragrance-free.” Cleansing twice a day is enough; more than that rarely helps and frequently harms. This single swap has more downstream impact than almost anything else in the routine.
Strategy 2: Build a prebiotic–probiotic–postbiotic stack
These three categories work differently. Prebiotics (inulin, oat beta-glucan) feed beneficial bacteria already on your skin. Probiotics (Lactobacillus fermentum, Bifidobacterium fermentum) introduce beneficial microbial byproducts. Postbiotics (fermented lysates, short-chain fatty acids) are the end products of bacterial activity and offer stability without the risks associated with live organisms.
Research published in Annals of Dermatology supports prebiotic and probiotic skincare as a non-invasive strategy to improve barrier function and reduce inflammatory skin responses.
If you want a clearer breakdown of how each one works—and which your skin actually needs—see our detailed guide on postbiotic vs prebiotic skincare.
Strategy 3: Moisturize with ceramide-rich formulas to support the barrier
A compromised skin barrier doesn’t just mean dryness. It means an unstable habitat for your microbial community.
Research shows that regular use of occlusive, ceramide-containing moisturizers reduces transepidermal water loss and creates more stable niche conditions for commensal bacteria — conditions they need to maintain consistent populations.
Ceramides, panthenol, squalane, and hyaluronic acid are the workhorses here. This isn’t about luxury; it’s about creating conditions where your microbiome can do its job.
If your barrier is already compromised, following a structured repair routine can accelerate recovery—see our complete guide to repairing a damaged skin barrier.
Strategy 4: Wear broad-spectrum SPF daily — for your microbes, too
UV radiation damages skin cells and disrupts their resident microbial populations. Beyond that, S. epidermidis’ UV-protective function — its ability to inhibit UV-damaged keratinocyte proliferation — only works when that commensal bacterium is present and thriving.
A broad-spectrum SPF 30 or higher, applied daily, protects the entire ecosystem. Not just collagen. Not just even skin tone. The microbiome needs this protection as much as the skin cells it lives on.
Strategy 5: Eat for your gut — because your skin microbiome feels it
The gut-skin axis is well-documented. Research cited in Microorganisms describes an active interplay between the gut and skin microbiota in conditions such as atopic dermatitis. Practically, that means consuming fermented foods (kimchi, kefir, live yogurt, miso) and fiber-rich prebiotic foods (oats, garlic, leeks, bananas), which support microbial diversity — not just in your gut but across the whole system.
Limiting ultra-processed foods and added sugar removes a key inflammatory driver that worsens dysbiosis at both sites.
Strategy 6: Sleep and stress — your microbiome follows a circadian rhythm
Skin biology is time-regulated; sebum production, cell turnover, DNA repair, and microbial activity all follow a 24-hour rhythm. Consistent sleep disruption impairs barrier repair and shifts the local environment on which commensal bacteria depend. Cortisol — the primary stress hormone — alters sebum composition and compromises tight junction proteins in the skin barrier.
Managing sleep and stress isn’t peripheral skincare advice. It’s foundational. Seven to nine hours of consistent sleep and regular stress reduction practices have measurable effects on skin microbial diversity.
Strategy 7: Ask harder questions before accepting antibiotics for skin conditions
Oral antibiotics cause significant, sometimes lasting changes to skin microbial communities, as the Science Translational Medicine study demonstrated. This doesn’t mean avoiding them when genuinely needed.
It means having informed conversations with your dermatologist about duration, necessity, and whether topical prebiotic or postbiotic alternatives might be appropriate. Antibiotic stewardship matters for your personal microbiome — not just for public health resistance patterns.
How to Restore Your Skin Microbiome Naturally — A Realistic Recovery Plan
If your microbiome has been disrupted — by antibiotics, harsh products, or years of over-washing — recovery is possible. But it takes time, consistency, and realistic expectations. Here’s what the science actually says.
How long does it realistically take for good bacteria to grow back?
It depends entirely on the severity and source of the disruption. After a single application of an antiseptic, commensals often rebound within hours or days.
After a full antibiotic course, the NIH-published Science Translational Medicine study found that antibiotic-resistant bacterial strains introduced during treatment persisted significantly long after the course ended — suggesting meaningful microbiome recovery can take several months, not days. Mild lifestyle-related disruption: 2 to 4 weeks. Post-antibiotic recovery: 3 to 6 months with consistent support.
The microbiome reset protocol — where to start
Strip your routine back to three products: one gentle, pH-balanced cleanser; one fragrance-free ceramide moisturizer; SPF. Nothing else for two weeks. No actives, no exfoliants, no new products. This creates stable baseline conditions — the right pH, adequate moisture, minimal antimicrobial stress — that allow the ecosystem to begin rebuilding. It’s not “doing nothing.” It’s removing the barriers to recovery. Then, slowly and one product at a time, reintroduce other elements over the following weeks.
Topical postbiotics as a recovery scaffold
Postbiotic ingredients — bifida ferment lysate, lactobacillus lysate, lactobacillus ferment — are shelf-stable, don’t carry live-organism infection risks, and are safe to apply even on compromised skin. Research published in Annals of Dermatology supports the use of postbiotic-containing skincare for barrier repair and microbiome stabilization.
Products containing these ingredients can be layered with a basic moisturizer during the reset phase without disrupting recovery — they scaffold the rebuilding process rather than challenging it.
Can oral probiotics help restore skin flora?
The evidence is growing but still nuanced. A 2024 review in Experimental Dermatology notes that probiotic interventions targeting the skin microbiome show promise, particularly with strains like Lactobacillus rhamnosus GG, Lactobacillus plantarum, and Bifidobacterium longum.
Results are cumulative and typically require 6 to 12 weeks of consistent supplementation. Oral probiotics work best as part of a broader strategy — not as a standalone fix for skin dysbiosis, but as a meaningful supporting element within a recovery protocol.
Why Korean Skincare Has Always Been Microbiome-Friendly
One of the most interesting things about K-beauty is that it arrived at microbiome science intuitively, decades before Western dermatology gave the concept a name. The philosophy was right — even if the vocabulary wasn’t there yet.
The fermentation tradition that science later validated
Korean skincare’s long history with fermented ingredients — galactomyces ferment filtrate, saccharomyces ferment, bifida ferment lysate — is rooted in a practical observation: fermented preparations worked better for the skin than their unfermented counterparts. Science now explains why.
According to research published by Beautipin, fermented ingredients contain postbiotic compounds — amino acids, organic acids, enzymes — that support the skin’s microbial balance and reinforce barrier function. The practice predated the science by generations.
Low-pH cleansers, layered hydration, and K-beauty habits anyone can adopt
K-beauty was pioneering the pH-balanced cleanser movement long before Western brands caught up. The multi-step layering approach — essence, serum, moisturizer — maintains the skin’s water activity (the moisture level commensal bacteria need to sustain stable populations).
Five habits anyone can adopt right now: switch to a low-pH cleanser, add a fermented essence after washing, layer lightweight hydration instead of relying on one heavy cream, look for bifida ferment lysate or galactomyces in serums, and make SPF non-negotiable. None of these requires an expensive K-beauty haul.
How to Choose Genuinely Microbiome-Friendly Products — Without Getting Misled
“Microbiome-friendly” is unregulated. Any brand can use it. That means the label tells you almost nothing — but the ingredient list tells you everything.
Ingredients worth seeking on labels (the supportive A-list)
Look for prebiotics — inulin, oat beta-glucan (Avena sativa), fructooligosaccharides, alpha-glucan oligosaccharide. Look for postbiotic actives — Lactobacillus ferment, bifida ferment, Galactomyces ferment filtrate, Saccharomyces ferment filtrate, Bifidobacterium ferment filtrate.
And look for barrier-supporting multi-taskers that create favorable conditions for the microbiome: ceramides, niacinamide, centella asiatica, panthenol, and squalane. The higher these appear in the INCI list, the more meaningful their concentration in the formula.
What to avoid — and how to recognize “microbiome washing”.
The ingredient avoidance list matters just as much. Denatured alcohol (alcohol denat.), sodium lauryl sulfate, triclosan, synthetic fragrance (parfum), methylisothiazolinone (MI), and polyhexamethylene biguanide (PHMB) all have documented disruptive effects on beneficial skin bacteria.
As for spotting misleading claims: if a product says it “completely restores your microbiome overnight” — that’s not how biology works. Real microbiome recovery takes weeks. A genuinely supportive product will be gentle, fragrance-free, and contain verifiable prebiotic or postbiotic ingredients listed prominently in the INCI.
Conclusion: What Is the Skin Microbiome and How to Protect It
Here’s what all of this comes down to: the healthiest skin isn’t the cleanest skin. It’s the most balanced.
Your skin microbiome has been doing its job — defending your barrier, training your immune cells, protecting against pathogens — since before you were old enough to have a skincare routine. The irony is that many of the habits modern culture promoted as good skincare have been systematically undermining it.
Over-cleansing, over-exfoliating, fragrance-loading, antibiotic-cycling. All of it chips away at an ecosystem that took a lifetime to build.
The good news? That ecosystem is resilient. It wants to recover. And for most people, the path back starts with one honest question: Is what I’m putting on my skin actually helping — or is it just making my skin work harder to compensate?
Start there. Pick one swap this week — a gentler cleanser, a fragrance-free moisturizer, a serum with bifida ferment lysate. You don’t need to rebuild the whole routine at once. The microbiome doesn’t work on dramatic overhauls; it works on consistent, sustained conditions that let it do what it’s already designed to do.
And if things aren’t improving after six weeks of simplification? See a board-certified dermatologist. Not every microbiome imbalance resolves with a skincare reset — and there’s no shame in getting clinical eyes on what’s happening.
Your skin is already doing most of the heavy lifting. The goal is to stop getting in its way.
Frequently Asked Questions: What Is the Skin Microbiome and How to Protect It
What Is The Microbiome Of The Human Skin?
The skin microbiome is the community of microorganisms—including bacteria, fungi, viruses, and mites—that live on and within the skin and support its health. These microbes help maintain the skin barrier, regulate immune responses, and prevent harmful pathogens from taking over.
According to Experimental Dermatology, over 1,000 bacterial species can be found on human skin, with variation by individual and environment. A balanced microbiome keeps skin stable and resilient. Supporting it with gentle skincare and consistent habits is essential for long-term skin health.
What Disrupts The Skin Microbiome?
The skin microbiome is disrupted by factors that damage microbial balance or the skin barrier, including antibiotics, harsh cleansers, over-exfoliation, UV exposure, and chronic stress. These disruptors alter skin pH, reduce beneficial bacteria, and create conditions that allow harmful microbes to thrive.
A Science Translational Medicine study shows that antibiotics can cause long-lasting changes in the microbiome. This imbalance increases sensitivity, breakouts, and inflammation. To prevent disruption, limit harsh products, protect your skin from UV exposure, and maintain a consistent, barrier-friendly routine.
What Kills The Good Bacteria On Your Skin?
Good skin bacteria are killed by antibacterial products, alcohol-based skincare, synthetic fragrance, aggressive exfoliation, and certain antibiotics. These factors act as broad-spectrum disruptors, removing beneficial microbes along with harmful ones and weakening the skin’s natural defense system.
Dermatology research confirms that this creates a recovery window during which opportunistic bacteria can overgrow. This leads to irritation, acne, and reduced skin resilience. To protect beneficial bacteria, avoid unnecessary antibacterial products and choose gentle, microbiome-supportive formulations.
How Do You Fix Your Skin Microbiome?
Fixing the skin microbiome means restoring balance through barrier repair and reducing microbial stress. This involves simplifying your routine to a gentle cleanser, a ceramide-rich moisturizer, and daily sunscreen while temporarily removing actives and irritants.
Research in Annals of Dermatology supports prebiotic and postbiotic skincare for improving microbial balance and reducing inflammation. A consistent routine allows beneficial bacteria to repopulate and stabilize. The key is patience—stick to simple, supportive skincare and avoid frequent changes.
How Do Koreans Keep Their Skin So Clear?
Clear skin in Korean skincare is largely supported by microbiome-friendly practices that maintain balance and hydration. Low-pH cleansers, fermented ingredients like galactomyces and bifida ferment, and consistent SPF use help preserve the skin barrier and beneficial bacteria.
These practices reduce irritation and support microbial stability over time. The result is smoother, more resilient skin with fewer disruptions. Adopting gentle, hydration-focused routines can help replicate these long-term benefits.
How Long Does It Take For Good Bacteria To Grow Back?
The time it takes for good skin bacteria to recover depends on the severity of microbiome disruption. Minor disruptions may recover within days, while antibiotic-related changes can take several months, as shown in Science Translational Medicine.
Recovery requires stable conditions that allow beneficial microbes to repopulate gradually. Slow recovery can lead to prolonged sensitivity and imbalance. Supporting your skin with a gentle, consistent routine can help restore balance within 2–6 months.
How Do You Restore The Skin Microbiome Naturally?
Restoring the skin microbiome naturally involves reducing disruption and supporting beneficial microbial growth through lifestyle and skincare. This includes using gentle, fragrance-free products, incorporating postbiotic ingredients, and consuming probiotic-rich and fiber-rich foods.
These steps help rebuild microbial diversity and strengthen the skin barrier over time. Consistent care improves hydration, reduces inflammation, and enhances resilience. Focus on long-term habits rather than quick fixes for sustainable microbiome recovery.
What Does An Unhealthy Skin Microbiome Look Like?
An unhealthy skin microbiome is characterized by imbalance, reduced diversity, and overgrowth of harmful microorganisms. This leads to symptoms like persistent acne, redness, sensitivity, eczema flares, and recurring infections.
A Journal of Clinical Medicine review highlights reduced microbial diversity as a key marker of diseased skin. These changes weaken the skin barrier and increase inflammation. Recognizing these signs early and switching to microbiome-friendly skincare can help restore balance and prevent conditions from worsening.
📋 Medical Disclaimer
For Educational Purposes Only: This article is written by Kousar Subhan, a Medical Writer and Researcher, and is intended for informational and educational purposes only. The content provided is based on scientific research, peer-reviewed studies, and dermatological literature available as of December 2025.
Not Medical Advice: The information in this article does not constitute medical advice, diagnosis, or treatment recommendations. It should not be used as a substitute for professional medical consultation, diagnosis, or treatment from a board-certified dermatologist or qualified healthcare provider.
Individual Results May Vary: Skin conditions, including hyperpigmentation, melasma, and UV-induced pigmentation, vary significantly between individuals based on genetics, skin type, hormonal factors, and environmental exposure.
Consult Your Healthcare Provider: Before starting any new skincare regimen, especially if you are pregnant, breastfeeding, have diagnosed skin conditions, are taking medications, have sensitive skin, or are undergoing dermatological treatments.
Product Safety: Always perform a patch test before using new skincare products. Discontinue use and consult a healthcare professional if you experience irritation or adverse reactions.