How to Repair a Damaged Skin Barrier: A 2026 Science Backed Guide
Your skin barrier is doing something extraordinary right now. Every single second, it’s blocking pollution, repelling bacteria, and holding moisture inside your body — all without a single conscious effort from you. But here’s the thing: up to 80% of skin sensitivity complaints seen by dermatologists trace back to one root cause — a compromised skin barrier.
Sound familiar?
If your skin suddenly stings when you apply your favorite serum, feels tight right after washing, or breaks out despite a “perfect” routine, your skin barrier may be crying out for help. And trust me, you are not alone.
This is especially common among people who use overly complex routines, such as those often seen in multi-step acne skincare.
The good news?
A damaged skin barrier is not permanent. With the right ingredients, a simplified routine, and a little patience, most people begin seeing meaningful improvement within 2 to 4 weeks, according to board-certified dermatologists.
In this guide, I’ll walk you through exactly how to repair your damaged skin barrier — from understanding what went wrong, to building a step-by-step recovery routine backed by clinical evidence.
Let’s get your skin feeling like itself again.
“The skin barrier is your body’s first and most important line of defense. When it’s compromised, everything else in your skincare routine becomes less effective.” — Dr. Geeta Yadav, Board-Certified Dermatologist.
What Is the Skin Barrier and Why Does It Matter?
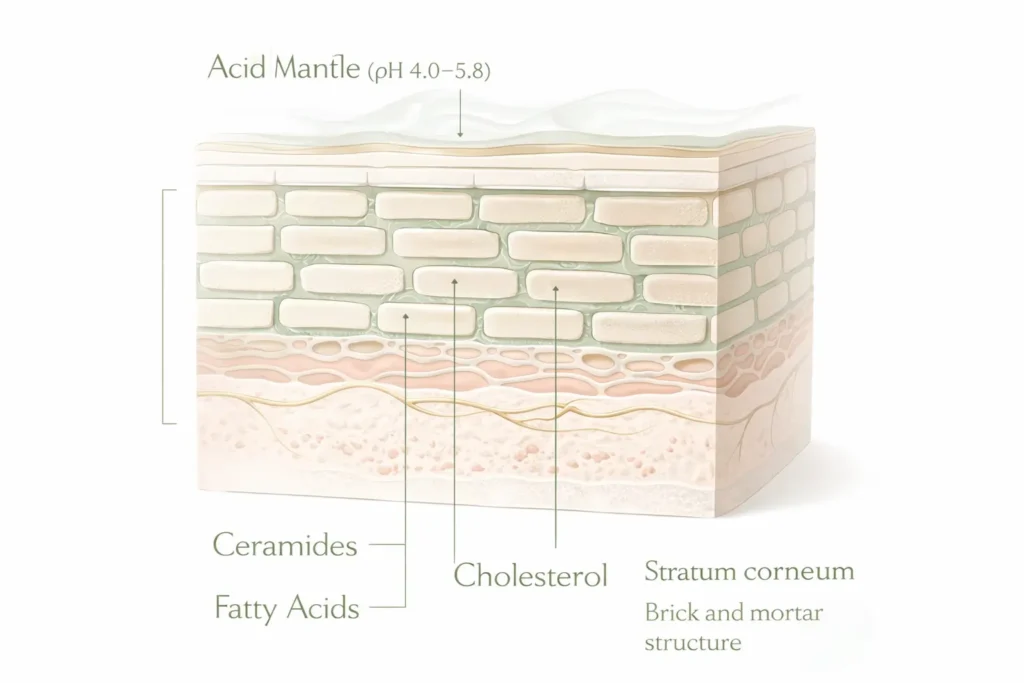
Think of your skin barrier — technically called the stratum corneum — as a brick wall. Corneocytes (flattened skin cells) are the bricks; a carefully organized lipid matrix is the mortar holding everything together. That lipid mortar is made of three components: ceramides (roughly 50%), cholesterol (25%), and free fatty acids (25%). The moment that ratio shifts, the wall starts to crumble.
Sitting just on top of this structure is what’s called the acid mantle: a thin, slightly acidic film with a pH of roughly 4.0 to 5.8. It may sound minor, but this acidic environment is what keeps harmful bacteria, fungi, and other pathogens from taking hold. Disrupt the pH — with an alkaline soap, an overly aggressive toner, or simply hot water — and you’ve left your skin open in ways you can’t immediately see.
The science here is well-established. A 2019 review in the Journal of Cosmetic Dermatology found that ceramide-containing moisturizers significantly reduce transepidermal water loss (TEWL) compared to standard hydrophilic creams — confirming that the specific lipid composition of the barrier is clinically meaningful, not just theoretical.
Beyond water retention, a healthy barrier regulates your skin’s immune response, blocks airborne irritants and UV-triggered free radicals, and keeps the natural moisture factor (NMF) — the collection of amino acids, lactic acid, and sugars that keep the surface hydrated — where it belongs. Honestly, it’s doing more work than most people give it credit for.
Signs Your Skin Barrier Is Damaged
Symptoms of a damaged barrier don’t always look dramatic. Sometimes they’re subtle enough that you attribute them to the wrong cause entirely. I’ve seen people chase “purging” when their skin was actually reacting to barrier damage caused by too many actives at once.
The most common signs to watch for:
| Symptom | What It Actually Signals |
| Tightness right after cleansing | Acid mantle disrupted; TEWL occurring faster than the skin can compensate |
| Stinging from products that used to feel fine | Lipid gaps in the stratum corneum allow irritants to penetrate deeper |
| Persistent dryness despite heavy moisturizer | Occlusion isn’t addressing the root lipid depletion |
| Sudden breakouts in an otherwise stable routine | Disrupted microbiome balance allows C. acnes to proliferate |
| Rough, sandpaper-like texture | Accelerated TEWL causes corneocyte irregularity on the surface |
| Redness, blotchiness, visible flushing | Skin’s inflammatory response is triggered by increased permeability |
| Dull, flat-looking skin | Compromised NMF causing light to scatter rather than reflect evenly |
One distinction I want to flag — because it confuses even seasoned skincare enthusiasts: damaged skin barrier and dry skin are not the same thing.
Dry skin is a skin type characterized by lower sebaceous activity. A damaged barrier is a condition. And it can happen to any skin type, including oily skin. In fact, oily-skinned people who over-strip their skin in the name of “controlling shine” are some of the most common barrier-damage cases I encounter in research contexts.
If your symptoms persist beyond six weeks despite gentle care — or you notice oozing, crusting, or intense inflammation — that’s your cue to see a board-certified dermatologist.
Conditions such as atopic dermatitis, rosacea, and psoriasis involve dysfunction of the skin barrier. The Cleveland Clinic’s guidance on skin barrier health is a solid starting point if you’re unsure which category you fall into.
What Causes a Damaged Skin Barrier?
The irony of modern skincare culture is that the damage often comes from the very products meant to improve your skin. Over-exfoliation is the most common culprit I see — people running glycolic acid and a retinoid in the same routine, then wondering why their skin feels raw.
Even popular treatments, like exfoliating scrubs, can worsen the problem when used too frequently. AHAs work by loosening the bonds between skin cells at the surface; when you’re using them too frequently, you’re essentially not allowing the lipid layer to stabilize between treatments.
But the causes go beyond your medicine cabinet:
Skincare Routine Mistakes
Using retinoids too aggressively (especially at the beginning), layering multiple low-pH acids, cleansing with hot water, and using fragrance-heavy products on sensitized skin — these are the most common routine errors I see. Alcohol-based toners deserve a special mention; ethanol is genuinely efficient at dissolving surface lipids, which is exactly why you don’t want it on an already-compromised barrier.
There’s good clinical documentation on this. L’Oréal Paris’s barrier science breakdown explains how even well-intentioned routines can disrupt the acid mantle’s integrity when active ingredients aren’t properly introduced.
Environmental and Lifestyle Factors
UV exposure directly breaks down structural lipids and proteins, which is one reason dermatologists are so insistent on SPF, even when it’s cloudy. Cold weather and dry indoor heating strip the surface moisture film faster than your skin can replace it.
Learn more about why daily sunscreen is essential in our detailed guide to sun protection and anti-aging skincare.
Chronic stress elevates cortisol, and cortisol has a fairly direct inhibitory effect on ceramide synthesis. Poor sleep disrupts the skin’s overnight repair cycle. Even low intake of omega-3 fatty acids and zinc can quietly compromise barrier integrity over months.
If you’re dealing with stress-triggered flare-ups, explore how stress affects pre-existing skin conditions and what dermatologists recommend to manage it.
Genetic and Medical Predispositions
Some people are working against their own biology here. Mutations in the filaggrin gene — more common in people of Northern European descent — directly impair the skin’s ability to form a competent barrier. Atopic dermatitis is, at its root, a filaggrin-related condition.
Diabetes alters skin pH in ways that compromise the acid mantle’s buffering capacity. Hormonal fluctuations — particularly around perimenopause — affect lipid production and barrier resilience in ways that aren’t talked about nearly enough.
How to Repair a Damaged Skin Barrier — Step-by-Step
This is the section I’d print out and tape to someone’s mirror. Not because it’s complicated — actually the opposite. The real challenge of barrier repair is psychological: it requires doing less when every skincare instinct tells you to do more.
| The Core Principle of Barrier Repair
• Remove the stressor. Add the building blocks. Let the skin’s own repair machinery do its job. • Your keratinocytes already know how to synthesize ceramides and fatty acids — they just need you to stop interrupting the process. |
Step 1 — Simplify Aggressively
The first and hardest step: stop using everything that could be causing or sustaining the damage. That means retinoids, AHAs (glycolic, lactic, mandelic), BHAs (salicylic acid), vitamin C in acidic forms (L-ascorbic acid above 10%), benzoyl peroxide, and physical scrubs. All of it. Cold turkey.
I know that’s hard to hear — especially if you’ve spent real money building a “sophisticated” active-heavy routine. But here’s the thing: none of those actives can do their job on compromised skin anyway. Your retinol isn’t anti-aging; it’s a barrier that can’t defend itself. Pare back to three steps — cleanse, treat, moisturize — and give your skin two to four weeks of recovery before reintroducing anything.
Step 2 — Rethink Your Cleanser
Your cleanser is either helping or hurting your barrier twice a day. A gentle, pH-balanced cleanser — ideally between pH 4.5 and 5.5 — preserves the acid mantle instead of destroying it. If you’re looking for options formulated specifically for delicate skin, consider switching to organic cleansers designed for sensitive skin.
Standard bar soaps often have a pH of 9 to 10, which is why dermatologists recommend alternatives like the Dove Sensitive Skin Beauty Bar for people with delicate or compromised skin.
That’s not a minor difference; it’s the equivalent of throwing alkaline bleach at a slightly acidic environment your skin has spent effort creating.
Use lukewarm water. Hot water dissolves the lipid film in under sixty seconds. Pat dry — never rub. Look for formulas free of sodium lauryl sulfate (SLS), fragrance, and alcohol. A good mid-range option that dermatologists frequently cite is CeraVe Hydrating Cleanser, which maintains pH balance and delivers ceramides and hyaluronic acid in a single wash.
Purexhc’s barrier repair guide covers cleanser selection in useful clinical detail, including why certain micellar formulas are more barrier-friendly than their sulfate-based counterparts.
Step 3 — Apply Barrier-Repairing Actives (Yes, There Are Some You Can Use)
Barrier repair isn’t entirely passive. There are a handful of ingredients that actively support the skin’s healing process — and they’re very different from the exfoliating and renewing actives you’re temporarily setting aside.
Apply these to damp skin — within sixty seconds of cleansing — when the concentration gradient effect pulls actives deeper into the stratum corneum. Let them absorb for two to three minutes before layering your moisturizer on top.
| “Niacinamide is one of the few actives we can confidently recommend during barrier recovery. It stimulates ceramide synthesis without exfoliating or altering skin pH — which is exactly the dual benefit compromised skin needs.”
— Dr. Geeta Yadav, Board-Certified Dermatologist |
That quote isn’t just clinical opinion — there’s a 2000 study in the British Journal of Dermatology demonstrating that niacinamide directly increases ceramide and fatty acid synthesis in the stratum corneum at concentrations as low as 2%. For damaged-barrier use, 4–5% is the sweet spot: effective, but not irritating.
Step 4 — Moisturize Strategically, Not Just Heavily
There’s a meaningful difference between slapping on a thick moisturizer and actually selecting one that feeds your skin’s lipid matrix. For barrier repair, you want a moisturizer that contains ceramides — specifically the three subtypes that match your skin’s own lipid composition: ceramide NP, ceramide AP, and ceramide EOP.
Add cholesterol and linoleic-acid-rich fatty acids to the formula, and you’re essentially handing your barrier the raw materials it needs to rebuild.
For severely dry patches — especially in cold or low-humidity climates — consider ‘slugging’ these areas at night: applying a thin layer of petrolatum (plain Vaseline works perfectly) as a final occlusive layer. Petrolatum doesn’t repair the barrier directly; it creates a near-impermeable seal that dramatically reduces TEWL while the skin heals underneath. It’s one of the most evidence-backed strategies in dermatology and costs almost nothing.
Step 5 — SPF Is Non-Negotiable During Repair
I’m going to be blunt about this one: skipping sunscreen while trying to repair your skin barrier is like trying to fill a bathtub with the drain open. UV exposure degrades ceramides and structural skin proteins every single day you’re outdoors — or near a window.
During the repair phase, choose a mineral sunscreen (zinc oxide or titanium dioxide) over chemical filters. Mineral formulas sit on the skin’s surface rather than penetrating it, which is much gentler on a barrier that’s already permeability-compromised.
The Best Ingredients for Skin Barrier Repair — What the Evidence Shows
I want to give you a clean, science-grounded reference here — because the ingredient space for barrier repair is genuinely crowded, and not everything that markets itself as ‘barrier-strengthening’ has the clinical backing to support that claim.
| Ingredient | What It Does for the Barrier | Best Used In | Safe During Repair? |
| Ceramides (NP, AP, EOP) | Directly replenish the lipid mortar of the stratum corneum; reduce TEWL | Moisturizers, night creams | Yes — essential |
| Niacinamide (2–10%) | Stimulates ceramide + fatty acid synthesis; reduces inflammation | Serums, toners, moisturizers | Yes — ideal |
| Panthenol (Pro-B5) | Supports ceramide production; soothes inflammation acutely | Serums, essences, moisturizers | Yes — excellent |
| Sunflower Seed Oil | Rich in linoleic acid — the omega-6 fatty acid depleted in damaged barriers | Facial oils, balms, serums | Yes — highly effective |
| Colloidal Oatmeal | Beta-glucan calms inflammatory response; reinforces barrier structure | Cleansers, moisturizers, masks | Yes — very soothing |
| Centella Asiatica | Reduces inflammatory cytokines; supports dermal collagen indirectly | Serums, toners, ampoules | Yes — safe and calming |
| Hyaluronic Acid (HA) | Draws moisture into the skin; best on damp skin sealed with occlusive | Serums, essences, mists | Yes — with occlusive |
| Petrolatum / Vaseline | Occlusive that dramatically reduces TEWL; creates a healing microenvironment | Overnight balms, slugging | Yes, particularly for night |
The science on ceramides specifically is robust. A study published in the Journal of Investigative Dermatology confirmed that physiological lipid mixtures — particularly those mimicking the skin’s own ceramide:cholesterol: fatty acid ratio — restore barrier function more effectively than single-ingredient approaches. This is why multi-ceramide formulas consistently outperform ceramide-only products in clinical comparisons.
A few things worth noting about plant oils: not all oils are created equal. Coconut oil is high in oleic acid, which — counterintuitively — has been shown in some studies to worsen barrier disruption in certain skin types, particularly eczema-prone skin. Linoleic-acid-rich oils like sunflower, rosehip, and evening primrose oil have genuine clinical support for barrier restoration.
What to Avoid When Your Skin Barrier Is Damaged
Just as important as what you add is what you stop. This might be the section that saves you the most time — because many people in barrier-repair mode inadvertently keep sabotaging their own progress.
| Ingredients to Pause Completely During Barrier Repair
• Retinoids (retinol, retinal, tretinoin, adapalene) — increase cell turnover, preventing the lipid layer from stabilizing • AHAs: glycolic acid, lactic acid, mandelic acid — low pH disrupts acid mantle further • BHAs: salicylic acid — oil-soluble; penetrates and destabilizes lipid layer directly • Benzoyl peroxide — potent oxidizer that damages healthy lipid structures • Vitamin C (L-ascorbic acid above 10%) — acidic pH is irritating on permeability-compromised skin • Physical scrubs, exfoliating brushes — mechanically strip healing corneocytes before they’ve consolidated • Fragrance and essential oils — even natural, these act as contact irritants on sensitized skin • Alcohol-based toners (ethanol, denatured alcohol) — strips surface lipids within minutes of application |
Beyond the ingredient list, lifestyle habits quietly sustain the damage. Very hot showers — I know, I know — dissolve the lipid film faster than any acid. Low-humidity environments (especially offices with aggressive air conditioning) accelerate TEWL hour after hour.
And if you’re someone who’s been managing stress with a 10-step routine as a coping mechanism, it’s worth noting that the cortisol from chronic stress directly inhibits ceramide synthesis. The routine that’s supposed to help might, in this case, be contributing to the problem.
Beautipin’s 2025 Korean skincare barrier-repair guide offers a practical breakdown of how to identify and remove routine stressors, including less-obvious culprits like overuse of alcohol-based sheet masks.
How Long Does It Take to Repair a Damaged Skin Barrier?
One of the questions I get most often — and the answer is genuinely: it depends. Not as a cop-out, but because the severity of the damage matters enormously here.
| Damage Level | Expected Repair Timeline with Consistent Gentle Care |
| Mild (1–2 weeks of over-exfoliation or a product reaction) | 2–4 weeks |
| Moderate (months of active-heavy routines, seasonal stress) | 4–8 weeks |
| Severe (chronic eczema flare, prescription-retinoid overuse, post-procedure) | 8–12+ weeks |
| Full lipid layer restoration (all damage levels) | 6–12 weeks of sustained barrier-focused care |
You’ll know your barrier is recovering when products stop stinging, skin stops feeling tight after cleansing, redness visibly reduces, and your complexion starts looking clearer and more naturally radiant. Dr. Yadav puts it plainly: “If your skin barrier is healthy, your skin will look clear and radiant” — and that shift, when it comes, is genuinely visible.
One thing worth managing: don’t panic, reintroduce your activities the moment you feel better. Give your barrier at least two weeks to feel genuinely comfortable before bringing anything back in — and when you do, start with one ingredient at a reduced frequency and watch closely.
The INKEY List’s damaged skin barrier resource has a useful guide to pacing the reintroduction of actives post-recovery — including a sequencing framework that dermatologists broadly agree with.
How to Maintain a Healthy Skin Barrier Long-Term
Once you’ve repaired the damage, the goal shifts from recovery to prevention. And honestly, the habits that maintain a healthy barrier aren’t dramatically different from the repair protocol — they’re just practiced at a lower intensity, consistently over time.
The Barrier-Protective Daily Routine (Morning and Evening)
Morning — what I’d call the protection-forward routine:
- Gentle, pH-balanced cleanser (skip this step entirely if your skin isn’t oily in the morning)
- Niacinamide serum at 4–5% concentration, applied to damp skin
- Ceramide-rich moisturizer — look for ceramides NP, AP, EOP on the label
- Mineral SPF 30+ — every day, rain or shine, home or office
Evening — the repair-and-replenish routine:
- Oil cleanser if wearing SPF or makeup; gentle second cleanse to follow
- Barrier serum (panthenol, centella, ceramide-focused)
- Rich barrier moisturizer — slightly heavier than your daytime formula
- Petrolatum on any particularly dry or compromised patches
Weekly: one gentle exfoliation pass with a PHA (polyhydroxy acid) or a very low-concentration lactic acid (5%) — once your barrier is fully repaired. PHAs are the gentlest chemical exfoliants available; they work at the very surface and don’t disrupt the lipid layer the way glycolic acid does.
For a broader view of where barrier repair fits within 2025–2026 skincare trends — including the rise of ‘skinimalism’ and minimalist barrier-first routines — Trustera’s analysis of top skincare trends is worth a read. The cultural shift toward fewer, better products is genuinely aligned with the evidence.
One last thing: your skin changes — seasonally, hormonally, and with age. A routine that worked brilliantly at 28 may need rethinking at 38. Revisit your routine quarterly. What you’re looking for isn’t a perfect formula you lock in forever; it’s a dynamic, responsive relationship with your own skin.
Final Thoughts
Repairing a damaged skin barrier comes down to one thing: removing what’s harming it and supplying what it needs to rebuild. That’s it. The rest is patience — which, I know, is easier said than done when your face is stinging, and your skin looks like it’s staging a revolt.
Start with the five-step protocol in the repair section. Lean hard on ceramides, niacinamide, and a pH-balanced cleanser. Drop the actives for a month. Wear SPF without exception. And resist the urge to ‘do more’ when things feel slow — the skin’s repair machinery is remarkably competent; it just needs you to stop interrupting it.
Most people see meaningful improvement within two to four weeks. Full recovery — the kind where you genuinely forget your barrier was ever compromised — typically takes six to twelve weeks. It’s worth every patient day of it.
Got questions about your specific routine or barrier damage situation? Drop them in the comments below — I read every one and answer with the evidence, not guesswork.
Frequently Asked Questions
How Can You Speed Up Skin Regeneration?
Prioritize sleep (skin synthesizes growth factors during deep sleep cycles), eat zinc- and omega-3-rich foods, keep skin consistently moisturized, and — once the barrier has stabilized — reintroduce retinoids at low frequency to accelerate keratinocyte turnover. Staying well-hydrated also supports dermal hyaluronic acid levels.
Is It Ever Too Late To Fix Your Skin?
Never. Clinical studies confirm that consistent use of ceramide-based moisturizers and SPF improves barrier function at any age. Recovery may take longer in mature skin due to slower cell turnover, but the barrier responds to proper care regardless of when you start.
What Is The Fastest Way To Heal A Damaged Skin Barrier?
Stop all exfoliating actives immediately. Switch to a pH-balanced cleanser, apply a ceramide-plus-niacinamide serum to damp skin twice daily, seal with a fragrance-free moisturizer, and use petrolatum on dry patches overnight. Most people notice measurable improvement within 7–14 days of this protocol.
How Long Does It Take For A Skin Barrier To Repair?
Mild damage: 2–4 weeks.
Moderate damage: 4–8 weeks.
Severe or chronic damage: 8–12 weeks or longer.
Full lipid layer restoration typically requires 6–12 weeks of sustained barrier-focused care with appropriate ingredients.
Can A Damaged Skin Barrier Repair On Its Own?
Yes — but only if you remove the cause of damage. Stop the stressors, and the skin’s keratinocytes will resume ceramide and lipid synthesis. Add supportive ingredients (ceramides, niacinamide) to speed up repair; ignore the root cause, and it can’t complete the cycle.
What Should You Not Use When Skin Barrier Is Damaged?
Avoid retinoids, AHAs, BHAs, benzoyl peroxide, fragrance, alcohol-based toners, physical scrubs, and high-pH soaps. These either accelerate cell turnover (blocking healing) or act as direct irritants that worsen TEWL. Resume them one at a time only after full recovery.
Can I Use Niacinamide If I Have A Damaged Skin Barrier?
Yes — niacinamide is one of the safest and most beneficial actives during barrier repair. It stimulates ceramide synthesis, reduces inflammation, and is non-acidic. Use a 4–5% concentration. It’s one of the few actives appropriate to keep using throughout the recovery phase.
What Oil Is Best For Skin Barrier Repair?
Sunflower seed oil — high in linoleic acid, the specific omega-6 fatty acid depleted in damaged barriers. Rosehip oil and evening primrose oil also work well. Avoid coconut oil on barrier-compromised or eczema-prone skin; its high oleic acid content can worsen disruption in some cases.
📋 Medical Disclaimer
For Educational Purposes Only: This article is written by Kousar Subhan, a Medical Writer and Researcher, and is intended for informational and educational purposes only. The content provided is based on scientific research, peer-reviewed studies, and dermatological literature available as of December 2025.
Not Medical Advice: The information in this article does not constitute medical advice, diagnosis, or treatment recommendations. It should not be used as a substitute for professional medical consultation, diagnosis, or treatment from a board-certified dermatologist or qualified healthcare provider.
Individual Results May Vary: Skin conditions, including hyperpigmentation, melasma, and UV-induced pigmentation, vary significantly between individuals based on genetics, skin type, hormonal factors, and environmental exposure.
Consult Your Healthcare Provider: Before starting any new skincare regimen, especially if you are pregnant, breastfeeding, have diagnosed skin conditions, are taking medications, have sensitive skin, or are undergoing dermatological treatments.
Product Safety: Always perform a patch test before using new skincare products. Discontinue use and consult a healthcare professional if you experience irritation or adverse reactions.
🛍️ Affiliate Disclosure
Amazon Associates Program: Glow Guide Hub participates in the Amazon Services LLC Associates Program. When you purchase through our Amazon affiliate links, we may earn a small commission at no extra cost to you.
Editorial Independence: Our affiliate relationships do not influence our content or recommendations. We only recommend products based on scientific research, clinical evidence, and genuine quality assessment.
Supporting Our Mission: Your purchases through affiliate links help us maintain this free, evidence-based educational resource. Thank you for your trust!